ℹ️ Skipped - page is already crawled
| Filter | Status | Condition | Details |
|---|---|---|---|
| HTTP status | PASS | download_http_code = 200 | HTTP 200 |
| Age cutoff | PASS | download_stamp > now() - 6 MONTH | 0.4 months ago |
| History drop | PASS | isNull(history_drop_reason) | No drop reason |
| Spam/ban | PASS | fh_dont_index != 1 AND ml_spam_score = 0 | ml_spam_score=0 |
| Canonical | PASS | meta_canonical IS NULL OR = '' OR = src_unparsed | Not set |
| Property | Value | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| URL | https://medlineplus.gov/ency/article/000259.htm | |||||||||
| Last Crawled | 2026-04-14 01:59:07 (10 days ago) | |||||||||
| First Indexed | 2016-07-17 04:10:33 (9 years ago) | |||||||||
| HTTP Status Code | 200 | |||||||||
| Content | ||||||||||
| Meta Title | Pseudomembranous colitis: MedlinePlus Medical Encyclopedia | |||||||||
| Meta Description | Pseudomembranous colitis refers to swelling or inflammation of the large intestine (colon) due to an overgrowth of Clostridioides difficile (C difficile) bacteria., Pseudomembranous colitis refers to swelling or inflammation of the large intestine (colon) due to an overgrowth of Clostridioides difficile (C difficile) bacteria. | |||||||||
| Meta Canonical | null | |||||||||
| Boilerpipe Text | Pseudomembranous colitis refers to swelling or inflammation of the large intestine (colon) due to an overgrowth of
Clostridioides difficile
(
C difficile
) bacteria.
This infection is a common cause of diarrhea after antibiotic use. Not all cases of diarrhea associated with antibiotic use are due to
C difficile
or will progress to pseudomembranous colitis.
The
C difficile
bacteria normally lives in the intestine. However, too much of these bacteria may grow when you take antibiotic medicines. The bacteria give off a strong toxin that causes inflammation and bleeding in the lining of the colon.
Any antibiotic can cause this condition. The medicines responsible for the problem most of the time are ampicillin, clindamycin, fluoroquinolones, and cephalosporins.
Health care providers in the hospital may pass this bacteria from one patient to another.
Pseudomembranous colitis is uncommon in children, and rare in infants. It is most often seen in people who are in the hospital. However, it is becoming more common in people who take antibiotics and are not in a hospital.
Risk factors include:
Older age
Antibiotic use
Use of medicines that weaken the immune system (such as chemotherapy medicines)
Recent surgery
History of pseudomembranous colitis
History of
ulcerative colitis
,
Crohn disease
, and inflammatory bowel disease (IBD).
C difficile
can happen in IBD patients even without taking antibiotics.
The following tests may be done:
Colonoscopy
or flexible sigmoidoscopy
Immunoassay for
C difficile toxin
in the stool
Polymerase chain reaction (PCR) for
C difficile
toxin in the stool
CT scan if complications are suspected
The antibiotic or other medicine causing the condition should be stopped. Fidaxomicin and vancomycin are most often used to treat the problem. Metronidazole is also effective, but it is no longer a first line choice in the US.
Electrolyte solutions
or fluids given through a vein may be needed to treat dehydration due to diarrhea. In rare cases, surgery is needed to treat infections that get worse or do not respond to antibiotics.
Long term antibiotics may be needed if the
C difficile
infection returns. A treatment called fecal microbiota transplant ("stool transplant") has also been effective for infections that come back.
Your provider may also suggest that you take probiotics if the infection returns.
An antibody treatment may be needed in patients with very high risk of recurrent
C difficile
to lessen the risk of recurrence.
The outlook is good in most cases, if there are no complications. However, up to 1 in 5 infections may return and need more treatment.
Complications may include:
Dehydration with electrolyte imbalance
Perforation of (hole through) the colon
Toxic megacolon
Death
Contact your provider if you have the following symptoms:
Any bloody stools (especially after taking antibiotics)
Five or more episodes of diarrhea per day for more than 1 to 2 days
Severe abdominal pain
Signs of dehydration
People who have had pseudomembranous colitis should tell their providers before taking antibiotics again. It is also very important to wash hands well to prevent passing the germ to other people. Alcohol sanitizers do not always work on
C difficile
.
Antibiotic-associated colitis; Colitis - pseudomembranous; Necrotizing colitis; C difficile - pseudomembranous; C diff
Gerding DN, Young VB. Donskey CJ.
Clostridiodes difficile
(formerly
Clostridium difficle
) infection. In: Bennett JE, Dolin R, Blaser MJ, eds.
Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases
. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 243.
Johnson S, Lavergne V, Skinner AM, et al. Clinical practice guideline by the Infectious Diseases Society of America (IDSA) and Society for Healthcare Epidemiology of America (SHEA): 2021 focused update guidelines on management of
clostridioides difficile
infection in adults.
Clin Infect Dis
. 2021; 73(5):e1029-e1044. PMID: 34164674
pubmed.ncbi.nlm.nih.gov/34164674/
.
Kelly CP, Khanna S. Antibiotic-associated diarrhea and
clostridioides difficile
infection. In: Feldman M, Friedman LS, Brandt LJ, eds.
Sleisenger and Fordtran's Gastrointestinal and Liver Disease
. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 112.
Wilcox MH, Dubberke ER. Clostridial and Clostridioides infections. In: Goldman L, Cooney KA, eds.
Goldman-Cecil Medicine
. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 271.
Updated by: Jenifer K. Lehrer, MD, Department of Gastroenterology, Aria - Jefferson Health Torresdale, Jefferson Digestive Diseases Network, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. | |||||||||
| Markdown | [Skip navigation](https://medlineplus.gov/ency/article/000259.htm#start)

An official website of the United States government
Here’s how you know
Here’s how you know

**Official websites use .gov**
A **.gov** website belongs to an official government organization in the United States.

**Secure .gov websites use HTTPS**
A **lock** ( Locked padlock icon) or **https://** means you’ve safely connected to the .gov website. Share sensitive information only on official, secure websites.
[](https://www.nih.gov/ "National Institutes of Health") [National Library of Medicine](https://www.nlm.nih.gov/)
[](https://medlineplus.gov/)
The navigation menu has been collapsed.
Menu
- [Health Topics](https://medlineplus.gov/healthtopics.html)
- [Drugs & Supplements](https://medlineplus.gov/druginformation.html)
- [Genetics](https://medlineplus.gov/genetics/)
- [Medical Tests](https://medlineplus.gov/lab-tests/)
- [Medical Encyclopedia](https://medlineplus.gov/encyclopedia.html)
- [About MedlinePlus](https://medlineplus.gov/about/)
Show Search
- [About MedlinePlus](https://medlineplus.gov/about/)
- [What's New](https://medlineplus.gov/whatsnew/)
- [Site Map](https://medlineplus.gov/sitemap.html)
- [Customer Support](https://support.nlm.nih.gov/knowledgebase/category/?id=CAT-01231&category=medlineplus&from=//medlineplus.gov/ency/article/000259.htm)
- [Health Topics](https://medlineplus.gov/healthtopics.html)
- [Drugs & Supplements](https://medlineplus.gov/druginformation.html)
- [Genetics](https://medlineplus.gov/genetics/)
- [Medical Tests](https://medlineplus.gov/lab-tests/)
- [Medical Encyclopedia](https://medlineplus.gov/encyclopedia.html)
[Español](https://medlineplus.gov/spanish/ency/article/000259.htm "Español")
You Are Here:
[Home](https://medlineplus.gov/) →
[Medical Encyclopedia](https://medlineplus.gov/encyclopedia.html) →
Pseudomembranous colitis
URL of this page: //medlineplus.gov/ency/article/000259.htm
# Pseudomembranous colitis
[](mailto:?subject=Pseudomembranous%20colitis%3A%20MedlinePlus%20Medical%20EncyclopediaLock&body=I%20found%20this%20information%20on%20MedlinePlus.gov%20and%20I'd%20like%20to%20share%20it%20with%20you%3A%0A%0Ahttps%3A%2F%2Fmedlineplus.gov%2Fency%2Farticle%2F000259.htm%3Futm_source%3Demail%26utm_medium%3Dshare%26utm_campaign%3Dmplus_share%0A%0AMedlinePlus%20\(https%3A%2F%2Fmedlineplus.gov\)%3A%20Trusted%20Health%20Information%20for%20you%0A%0ATo%20get%20updates%20by%20email%20when%20new%20information%20becomes%20available%20on%20MedlinePlus%2C%20sign%20up%20at%20https%3A%2F%2Fmedlineplus.gov%2Flistserv.html. "Email this page to a friend") [](https://medlineplus.gov/ency/article/000259.htm "Print") [](https://medlineplus.gov/ency/article/000259.htm "Facebook") [](https://medlineplus.gov/ency/article/000259.htm "X") [](https://medlineplus.gov/ency/article/000259.htm "Pinterest")
To use the sharing features on this page, please enable JavaScript.
Pseudomembranous colitis refers to swelling or inflammation of the large intestine (colon) due to an overgrowth of *Clostridioides difficile* (*C difficile*) bacteria.
This infection is a common cause of diarrhea after antibiotic use. Not all cases of diarrhea associated with antibiotic use are due to *C difficile* or will progress to pseudomembranous colitis.
## Causes
Expand Section
The *C difficile* bacteria normally lives in the intestine. However, too much of these bacteria may grow when you take antibiotic medicines. The bacteria give off a strong toxin that causes inflammation and bleeding in the lining of the colon.
Any antibiotic can cause this condition. The medicines responsible for the problem most of the time are ampicillin, clindamycin, fluoroquinolones, and cephalosporins.
Health care providers in the hospital may pass this bacteria from one patient to another.
Pseudomembranous colitis is uncommon in children, and rare in infants. It is most often seen in people who are in the hospital. However, it is becoming more common in people who take antibiotics and are not in a hospital.
Risk factors include:
- Older age
- Antibiotic use
- Use of medicines that weaken the immune system (such as chemotherapy medicines)
- Recent surgery
- History of pseudomembranous colitis
- History of [ulcerative colitis](https://medlineplus.gov/ency/article/000250.htm), [Crohn disease](https://medlineplus.gov/ency/article/000249.htm), and inflammatory bowel disease (IBD). *C difficile* can happen in IBD patients even without taking antibiotics.
## Symptoms
Expand Section
Symptoms include:
- [Abdominal cramps](https://medlineplus.gov/ency/article/003120.htm) (mild to severe)
- [Bloody stools](https://medlineplus.gov/ency/article/003130.htm)
- Fever
- Urge to have a bowel movement
- Watery [diarrhea](https://medlineplus.gov/ency/article/003126.htm) (often 5 to 10 times per day)
## Exams and Tests
Expand Section
The following tests may be done:
- [Colonoscopy](https://medlineplus.gov/ency/article/003886.htm) or flexible sigmoidoscopy
- Immunoassay for [C difficile toxin](https://medlineplus.gov/ency/article/003590.htm) in the stool
- Polymerase chain reaction (PCR) for *C difficile* toxin in the stool
- CT scan if complications are suspected
## Treatment
Expand Section
The antibiotic or other medicine causing the condition should be stopped. Fidaxomicin and vancomycin are most often used to treat the problem. Metronidazole is also effective, but it is no longer a first line choice in the US.
[Electrolyte solutions](https://medlineplus.gov/ency/article/002350.htm) or fluids given through a vein may be needed to treat dehydration due to diarrhea. In rare cases, surgery is needed to treat infections that get worse or do not respond to antibiotics.
Long term antibiotics may be needed if the *C difficile* infection returns. A treatment called fecal microbiota transplant ("stool transplant") has also been effective for infections that come back.
Your provider may also suggest that you take probiotics if the infection returns.
An antibody treatment may be needed in patients with very high risk of recurrent *C difficile* to lessen the risk of recurrence.
## Outlook (Prognosis)
Expand Section
The outlook is good in most cases, if there are no complications. However, up to 1 in 5 infections may return and need more treatment.
## Possible Complications
Expand Section
Complications may include:
- Dehydration with electrolyte imbalance
- Perforation of (hole through) the colon
- [Toxic megacolon](https://medlineplus.gov/ency/article/000248.htm)
- Death
## When to Contact a Medical Professional
Expand Section
Contact your provider if you have the following symptoms:
- Any bloody stools (especially after taking antibiotics)
- Five or more episodes of diarrhea per day for more than 1 to 2 days
- Severe abdominal pain
- Signs of dehydration
## Prevention
Expand Section
People who have had pseudomembranous colitis should tell their providers before taking antibiotics again. It is also very important to wash hands well to prevent passing the germ to other people. Alcohol sanitizers do not always work on *C difficile*.
## Alternative Names
Expand Section
Antibiotic-associated colitis; Colitis - pseudomembranous; Necrotizing colitis; C difficile - pseudomembranous; C diff
## Images
Expand Section
- 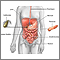[Digestive system](https://medlineplus.gov/ency/imagepages/1090.htm)
- 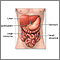[Digestive system organs](https://medlineplus.gov/ency/imagepages/8710.htm)
## References
Expand Section
Gerding DN, Young VB. Donskey CJ. *Clostridiodes difficile* (formerly *Clostridium difficle*) infection. In: Bennett JE, Dolin R, Blaser MJ, eds. *Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases*. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 243.
Johnson S, Lavergne V, Skinner AM, et al. Clinical practice guideline by the Infectious Diseases Society of America (IDSA) and Society for Healthcare Epidemiology of America (SHEA): 2021 focused update guidelines on management of *clostridioides difficile* infection in adults. *Clin Infect Dis*. 2021; 73(5):e1029-e1044. PMID: 34164674 [pubmed.ncbi.nlm.nih.gov/34164674/](https://pubmed.ncbi.nlm.nih.gov/34164674/).
Kelly CP, Khanna S. Antibiotic-associated diarrhea and *clostridioides difficile* infection. In: Feldman M, Friedman LS, Brandt LJ, eds. *Sleisenger and Fordtran's Gastrointestinal and Liver Disease*. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 112.
Wilcox MH, Dubberke ER. Clostridial and Clostridioides infections. In: Goldman L, Cooney KA, eds. *Goldman-Cecil Medicine*. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 271.
## Review Date 5/14/2024
Expand Section
Updated by: Jenifer K. Lehrer, MD, Department of Gastroenterology, Aria - Jefferson Health Torresdale, Jefferson Digestive Diseases Network, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
Learn how to cite this page
## Related MedlinePlus Health Topics
Expand Section
- [Antibiotics](https://medlineplus.gov/antibiotics.html)
- [C. diff Infections](https://medlineplus.gov/cdiffinfections.html)
## Related MedlinePlus Health Topics
- [Antibiotics](https://medlineplus.gov/antibiotics.html)
- [C. diff Infections](https://medlineplus.gov/cdiffinfections.html)
## Images
- [Digestive system](https://medlineplus.gov/ency/imagepages/1090.htm)
- [Digestive system organs](https://medlineplus.gov/ency/imagepages/8710.htm)
## Was this page helpful?
Yes
No
Thank you for your feedback\!
[](https://accreditnet.urac.org/directory/#/certification/HCP010004/info)
Health Content Provider
06/01/2028
[A.D.A.M., Inc. is accredited by URAC](), for Health Content Provider (www.urac.org). URAC's [accreditation program]() is an independent audit to verify that A.D.A.M. follows rigorous standards of quality and accountability. A.D.A.M. is among the first to achieve this important distinction for online health information and services. Learn more about A.D.A.M.'s [editorial policy, editorial process](), and [privacy policy]().
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. No warranty of any kind, either expressed or implied, is made as to the accuracy, reliability, timeliness, or correctness of any translations made by a third-party service of the information provided herein into any other language.
© 1997- 2026 A.D.A.M., a business unit of Ebix, Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
All content on this site including text, images, graphics, audio, video, data, metadata, and compilations is protected by copyright and other intellectual property laws. You may view the content for personal, noncommercial use. Any other use requires prior written consent from Ebix. You may not copy, reproduce, distribute, transmit, display, publish, reverse-engineer, adapt, modify, store beyond ordinary browser caching, index, mine, scrape, or create derivative works from this content. You may not use automated tools to access or extract content, including to create embeddings, vectors, datasets, or indexes for retrieval systems. Use of any content for training, fine-tuning, calibrating, testing, evaluating, or improving AI systems of any kind is prohibited without express written consent. This includes large language models, machine learning models, neural networks, generative systems, retrieval-augmented systems, and any software that ingests content to produce outputs. Any unauthorized use of the content including AI-related use is a violation of our rights and may result in legal action, damages, and statutory penalties to the fullest extent permitted by law. Ebix reserves the right to enforce its rights through legal, technological, and contractual measures.
[](https://www.adam.com/about)
- [About MedlinePlus](https://medlineplus.gov/about/)
- [What's New](https://medlineplus.gov/whatsnew/)
- [Site Map](https://medlineplus.gov/sitemap.html)
- [Customer Support](https://support.nlm.nih.gov/knowledgebase/category/?id=CAT-01231&category=medlineplus&from=httpsundefined)
- [Subscribe to RSS](https://medlineplus.gov/rss.html)
- [Connect with NLM](https://www.nlm.nih.gov/socialmedia/index.html)
- [NLM Web Policies](https://www.nlm.nih.gov/web_policies.html)
- [Copyright](https://medlineplus.gov/about/using/usingcontent/)
- [Accessibility](https://medlineplus.gov/accessibility.html)
- [Guidelines for Links](https://medlineplus.gov/about/using/criteria/)
- [Viewers & Players](https://medlineplus.gov/plugins.html)
- [HHS Vulnerability Disclosure](https://www.hhs.gov/vulnerability-disclosure-policy/index.html)
- [MedlinePlus Connect for EHRs](https://medlineplus.gov/medlineplus-connect/)
- [For Developers](https://medlineplus.gov/about/developers/)
[National Library of Medicine](https://www.nlm.nih.gov/) 8600 Rockville Pike, Bethesda, MD 20894 [U.S. Department of Health and Human Services](https://www.hhs.gov/) [National Institutes of Health](https://www.nih.gov/)
[](https://medlineplus.gov/ency/article/000259.htm#top "Return to top") | |||||||||
| Readable Markdown | Pseudomembranous colitis refers to swelling or inflammation of the large intestine (colon) due to an overgrowth of *Clostridioides difficile* (*C difficile*) bacteria.
This infection is a common cause of diarrhea after antibiotic use. Not all cases of diarrhea associated with antibiotic use are due to *C difficile* or will progress to pseudomembranous colitis.
The *C difficile* bacteria normally lives in the intestine. However, too much of these bacteria may grow when you take antibiotic medicines. The bacteria give off a strong toxin that causes inflammation and bleeding in the lining of the colon.
Any antibiotic can cause this condition. The medicines responsible for the problem most of the time are ampicillin, clindamycin, fluoroquinolones, and cephalosporins.
Health care providers in the hospital may pass this bacteria from one patient to another.
Pseudomembranous colitis is uncommon in children, and rare in infants. It is most often seen in people who are in the hospital. However, it is becoming more common in people who take antibiotics and are not in a hospital.
Risk factors include:
- Older age
- Antibiotic use
- Use of medicines that weaken the immune system (such as chemotherapy medicines)
- Recent surgery
- History of pseudomembranous colitis
- History of [ulcerative colitis](https://medlineplus.gov/ency/article/000250.htm), [Crohn disease](https://medlineplus.gov/ency/article/000249.htm), and inflammatory bowel disease (IBD). *C difficile* can happen in IBD patients even without taking antibiotics.
The following tests may be done:
- [Colonoscopy](https://medlineplus.gov/ency/article/003886.htm) or flexible sigmoidoscopy
- Immunoassay for [C difficile toxin](https://medlineplus.gov/ency/article/003590.htm) in the stool
- Polymerase chain reaction (PCR) for *C difficile* toxin in the stool
- CT scan if complications are suspected
The antibiotic or other medicine causing the condition should be stopped. Fidaxomicin and vancomycin are most often used to treat the problem. Metronidazole is also effective, but it is no longer a first line choice in the US.
[Electrolyte solutions](https://medlineplus.gov/ency/article/002350.htm) or fluids given through a vein may be needed to treat dehydration due to diarrhea. In rare cases, surgery is needed to treat infections that get worse or do not respond to antibiotics.
Long term antibiotics may be needed if the *C difficile* infection returns. A treatment called fecal microbiota transplant ("stool transplant") has also been effective for infections that come back.
Your provider may also suggest that you take probiotics if the infection returns.
An antibody treatment may be needed in patients with very high risk of recurrent *C difficile* to lessen the risk of recurrence.
The outlook is good in most cases, if there are no complications. However, up to 1 in 5 infections may return and need more treatment.
Complications may include:
- Dehydration with electrolyte imbalance
- Perforation of (hole through) the colon
- [Toxic megacolon](https://medlineplus.gov/ency/article/000248.htm)
- Death
Contact your provider if you have the following symptoms:
- Any bloody stools (especially after taking antibiotics)
- Five or more episodes of diarrhea per day for more than 1 to 2 days
- Severe abdominal pain
- Signs of dehydration
People who have had pseudomembranous colitis should tell their providers before taking antibiotics again. It is also very important to wash hands well to prevent passing the germ to other people. Alcohol sanitizers do not always work on *C difficile*.
Antibiotic-associated colitis; Colitis - pseudomembranous; Necrotizing colitis; C difficile - pseudomembranous; C diff
Gerding DN, Young VB. Donskey CJ. *Clostridiodes difficile* (formerly *Clostridium difficle*) infection. In: Bennett JE, Dolin R, Blaser MJ, eds. *Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases*. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 243.
Johnson S, Lavergne V, Skinner AM, et al. Clinical practice guideline by the Infectious Diseases Society of America (IDSA) and Society for Healthcare Epidemiology of America (SHEA): 2021 focused update guidelines on management of *clostridioides difficile* infection in adults. *Clin Infect Dis*. 2021; 73(5):e1029-e1044. PMID: 34164674 [pubmed.ncbi.nlm.nih.gov/34164674/](https://pubmed.ncbi.nlm.nih.gov/34164674/).
Kelly CP, Khanna S. Antibiotic-associated diarrhea and *clostridioides difficile* infection. In: Feldman M, Friedman LS, Brandt LJ, eds. *Sleisenger and Fordtran's Gastrointestinal and Liver Disease*. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 112.
Wilcox MH, Dubberke ER. Clostridial and Clostridioides infections. In: Goldman L, Cooney KA, eds. *Goldman-Cecil Medicine*. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 271.
Updated by: Jenifer K. Lehrer, MD, Department of Gastroenterology, Aria - Jefferson Health Torresdale, Jefferson Digestive Diseases Network, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. | |||||||||
| ML Classification | ||||||||||
| ML Categories |
Raw JSON{
"/Health": 997,
"/Health/Health_Conditions": 968,
"/Health/Health_Conditions/GERD_and_Digestive_Disorders": 664
} | |||||||||
| ML Page Types |
Raw JSON{
"/Article": 997,
"/Article/Definitions": 840
} | |||||||||
| ML Intent Types |
Raw JSON{
"Informational": 999
} | |||||||||
| Content Metadata | ||||||||||
| Language | en | |||||||||
| Author | null | |||||||||
| Publish Time | not set | |||||||||
| Original Publish Time | 2016-07-17 04:10:33 (9 years ago) | |||||||||
| Republished | No | |||||||||
| Word Count (Total) | 1,395 | |||||||||
| Word Count (Content) | 713 | |||||||||
| Links | ||||||||||
| External Links | 14 | |||||||||
| Internal Links | 30 | |||||||||
| Technical SEO | ||||||||||
| Meta Nofollow | No | |||||||||
| Meta Noarchive | No | |||||||||
| JS Rendered | Yes | |||||||||
| Redirect Target | null | |||||||||
| Performance | ||||||||||
| Download Time (ms) | 62 | |||||||||
| TTFB (ms) | 62 | |||||||||
| Download Size (bytes) | 8,794 | |||||||||
| Shard | 34 (laksa) | |||||||||
| Root Hash | 14962761832352801234 | |||||||||
| Unparsed URL | gov,medlineplus!/ency/article/000259.htm s443 | |||||||||